The Perimenopause Roller Coaster: What to Expect, Why It Happens, and How to Navigate It
At some point in your late 30s or 40s, things start to feel… different. Your cycle shifts. Your mood surprises you. Sleep gets unpredictable. And just when you think you’ve figured it out—everything changes again.
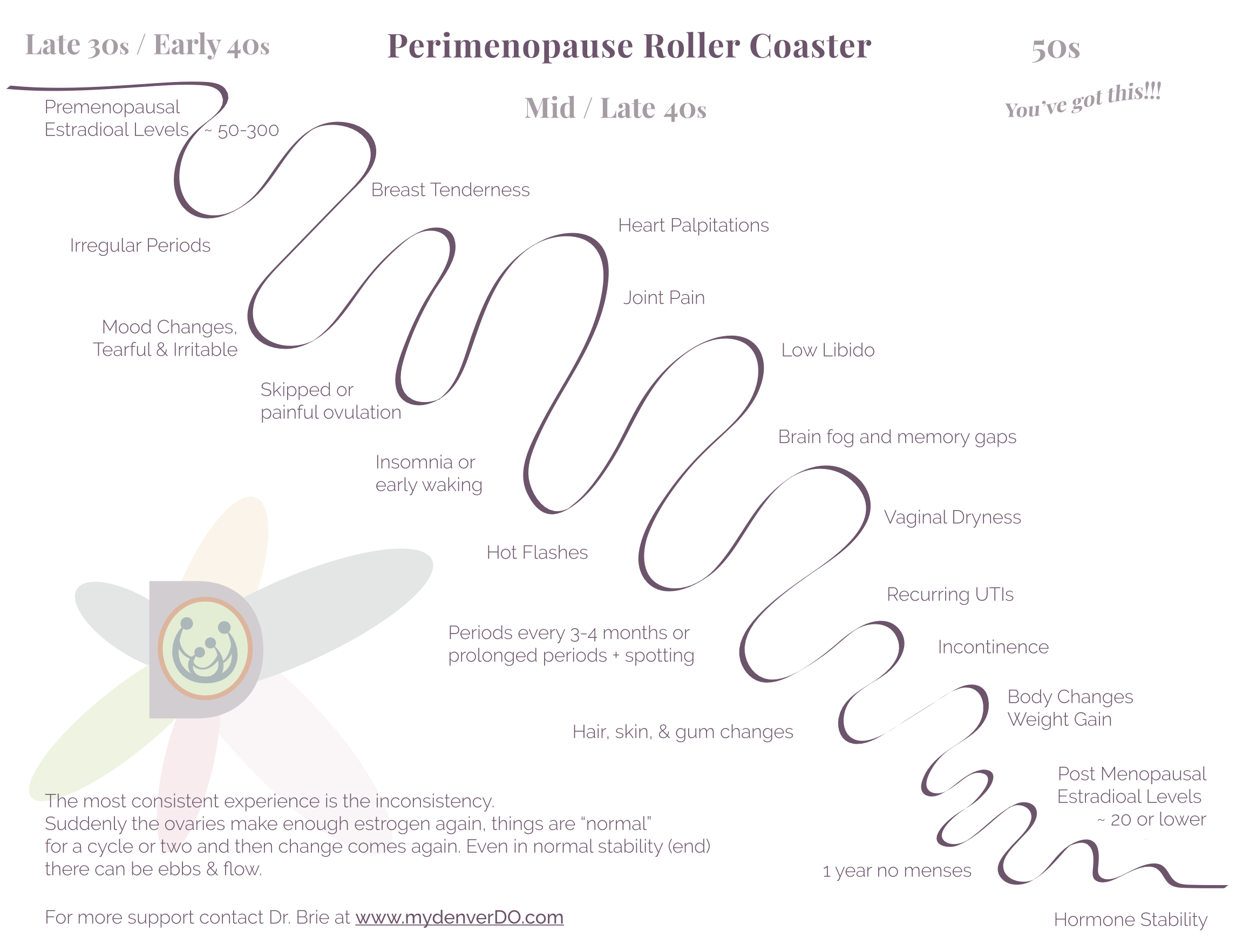
Welcome to perimenopause. Not a straight line, but a roller coaster.
It Starts Subtly (Late 30s to Early 40s)
Before anything looks “official,” your hormones begin to fluctuate behind the scenes.
Estrogen (estradiol) is still present—often in normal ranges (~50–300)—but it’s no longer steady. That variability is what drives early symptoms like:
Irregular periods
Mood changes (tearful, irritable, reactive)
Subtle cycle shifts you can’t quite predict
At this stage, many women feel dismissed because labs can look “normal.” But the experience isn’t about static levels—it’s about fluctuation.
The Middle Phase: Where Things Get Unpredictable
As you move into your mid to late 40s, the swings get wider—and more noticeable.
Ovulation becomes inconsistent, which can show up as:
Skipped or painful ovulation
Breast tenderness
Periods that come early, late, or not at all
Sleep often takes a hit:
Insomnia
Early waking (that 3am wide-awake feeling)
And then come the hallmark symptoms:
Hot flashes
Heart palpitations
Joint pain
Noticeable dips in libido
Your cycle might stretch out—periods every 3–4 months—or linger longer than usual with spotting.
This is often the most frustrating phase because it lacks predictability. You can feel completely normal one month and completely off the next.
The Mental Load: Brain Fog Is Real
As hormones continue shifting, many women notice cognitive changes:
Brain fog
Memory gaps
Difficulty focusing
This isn’t a lack of discipline—it’s biology. Estrogen plays a role in brain function, and when it fluctuates, so does mental clarity.
The Physical Shifts
Later in perimenopause, the changes extend beyond cycles and mood:
Vaginal dryness
Recurring UTIs
Incontinence
Skin, hair, and even gum changes
Weight gain or body composition shifts
These changes are often interconnected—driven by declining and fluctuating estrogen, plus changes in muscle mass, metabolism, and tissue integrity.
The Final Transition: Menopause
Menopause is defined simply: one full year without a period.
At that point:
Estradiol levels drop to ~20 or lower
Hormones stabilize—but at a new baseline
For many, symptoms like hot flashes may continue for a time, but the chaos of fluctuation begins to settle.
The Truth No One Talks About
The most consistent part of perimenopause is the inconsistency.
You may feel like yourself again for a cycle or two—only for symptoms to return. That doesn’t mean you’re going backward. It means your body is still transitioning.
Even at the end, there can be ebbs and flows.
So What Do You Do With All This?
You don’t fight the roller coaster—you learn how to ride it.
That means:
Understanding what’s happening in your body
Supporting sleep, stress, and nervous system health
Looking at root causes—not just symptoms
Getting guidance that takes your full picture into account
Because this phase isn’t just about hormones. It’s about how your entire system adapts.
You’re Not Alone in This
If you’ve been feeling off, out of sync, or like your body is changing without a clear reason—you’re not imagining it.
And you don’t have to navigate it blindly.
With the right support, perimenopause can shift from confusing and reactive… to something you understand, manage, and move through with clarity.
If you’re looking for personalized support, reach out to us to start a more informed, grounded approach to this transition.